Factors Associated with Better or Worse Sexual Well-Being After Breast Cancer
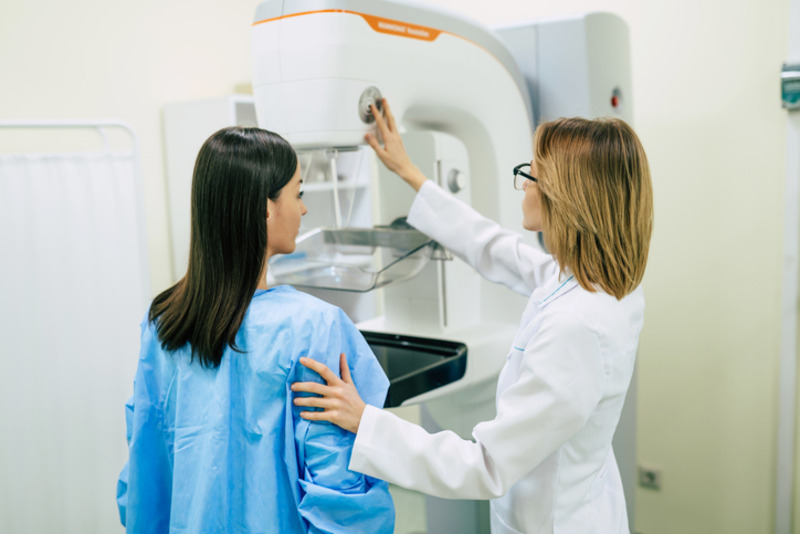
Breast cancer is the most common type of cancer among women. However, advancements in treatments have improved the survival rate and increased the average life expectancy of women with breast cancer. As such, it is more important than ever to strive to improve the sexual well-being and overall quality of life of women after a breast cancer diagnosis.
This type of cancer can have a particularly negative impact on a woman’s sexual health because its treatments (i.e., endocrine (hormone) therapy and chemotherapy) can lead to reduced lubrication, decreased sexual desire, and vaginal pain. What’s more, changes in and/or the removal of the breasts may impact breast cancer survivors psychologically, potentially causing decreased self-esteem or negative changes in one’s body image.
While past studies have focused on the sexual function (or dysfunction) of women after breast cancer and its treatment, few have explored the sexual well-being of these individuals. This distinction is important because the World Health Organization (WHO) defines sexual well-being as “a state of physical, emotional, mental, and social well-being in relation to sexuality, not merely the absence of diseases, dysfunction, or infirmity.”
Therefore, a recent study aimed to identify factors that may have a positive or negative influence on a woman’s sexual well-being after breast cancer. To do this, the researchers developed an online questionnaire to measure breast cancer survivors’ sexual well-being at the time of their diagnosis and again one year later.
The questionnaire also asked about the participants’ age, body mass index (BMI), menopausal status, type of surgery (breast conserving, mastectomy, or reconstruction), change in psychological well-being, family status, experience with endocrine therapy, and whether or not they had neoadjuvant (before surgery) or adjuvant (after surgery) chemotherapy.
A total of 204 patients who had been treated for breast cancer at the Academic Breast Cancer Center, Erasmus University Medical Center in Rotterdam between October 2015 and March 2022 completed the questionnaire at both timepoints. The average age of these participants was 51.7 years, and their average sexual well-being score at baseline was 64.3 (on a scale from 0 to 100 with higher scores indicating better sexual well-being).
The researchers found that a few factors were related to changes in the women’s sexual well-being one year after diagnosis. First, having a BMI > 30 at the start of the study had a significant negative impact on a woman’s change in sexual well-being. On the other hand, change in psychological well-being had a positive effect on change in sexual well-being. Lastly, breast reconstruction and mastectomy (the removal of the breast or breasts) had a significantly more positive effect on a woman’s sexual well-being than lumpectomy (a surgery in which just the tumor and a small amount of the surrounding area are removed).
Menopausal status and whether or not the women had endocrine therapy did not appear to influence their sexual well-being a year later. Nevertheless, the results of this study indicate that there is room to improve the sexual well-being of women after a breast cancer diagnosis, and more support and resources from health care providers and mental health professionals may be beneficial.
For more information on this topic, please read these publications from the ISSM Journals: The Journal of Sexual Medicine, Sexual Medicine Reviews, and Sexual Medicine Open Access:
Sexual well-being in patients with early-stage breast cancer at 1- and 2-year follow-up
Sexual dysfunctions in breast cancer patients: evidence in context
Low Sexual Desire in Breast Cancer Survivors and Patients: A Review
Preparing for Survivorship: Quality of Life in Breast Cancer Survivors
References:
Huberts, A.S., Clarijs, M.E., Pastoor, H., van Rosmalen, M., & Koppert, L.B. (2023). Sexual well-being in patients with early-stage breast cancer at 1-and 2-year follow-up. The Journal of Sexual Medicine, 20(4), 507-514. https://doi.org/10.1093/jsxmed/qdad007
You may also be interested in...
Other Popular Articles

What Is the Average Penis Size?
If you have ever wondered how your penis compares to others in terms of size, you are not alone. Many men are curious to know how their penises stack up compared to the average. Unfortunately, general curiosity can sometimes give way to full-on obsession and anxiety about penis size. This can be an unhealthy and often unnecessary fixation, especially because most men who think their penises are too small have perfectly normal-sized penises.

What Is Jelqing, and Does It Actually Work?
The term “jelqing” refers to a set of penis stretching exercises that some believe can make the penis bigger. Although the practice has gained attention and popularity in blogs and internet forums in recent years, there is no scientific evidence that it is an effective way to permanently increase the size of one’s penis. In fact, in some cases, jelqing may actually cause damage to the penis, so it is a good idea to get all the facts before setting off to try it.

What Is Sensate Focus and How Does It Work?
Sensate focus is a technique used to improve intimacy and communication between partners around sex, reduce sexual performance anxiety, and shift away from ingrained, goal-oriented sexual patterns that may not be serving a couple.

Can Sex Reduce Menstrual Cramps?
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Having sex while you experience menstrual cramps is healthy and can provide significant benefits. While it might not be the first activity that comes to mind when your PMS or period cramping begins, many people enjoy sex to reduce menstrual cramps, experience increased pleasure and benefit from other advantages. Learn more about having sex while menstrual cramps are happening and how it can help your body.

How Long Does It Take the Average Man to Ejaculate?
On average, it takes a man between 5 to 7 minutes to orgasm and ejaculate during sexual intercourse.

Can Sex Throw off Your Vaginal pH Balance?
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Your vagina is a pretty powerful organ. It is a pathway for menstrual blood and babies. It also is a main player in sexual intercourse. You might hear about your vagina’s pH and worry that yours is at risk. Here’s what to know about vaginal pH, including the impacts sex could have.
You are prohibited from using or uploading content you accessed through this website into external applications, bots, software, or websites, including those using artificial intelligence technologies and infrastructure, including deep learning, machine learning and large language models and generative AI.

